Understanding Leukoplakia
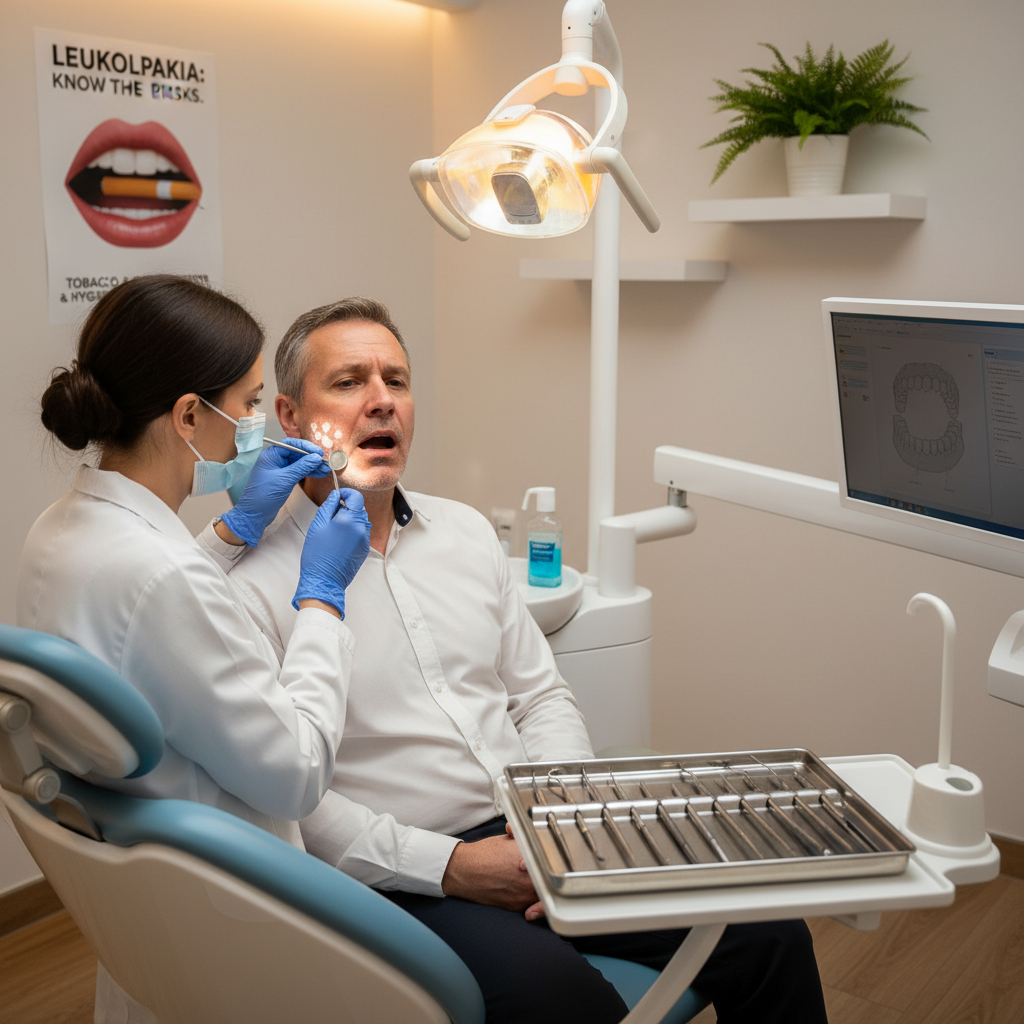
Leukoplakia presents as white patches on the oral mucosa, with a risk of progression to oral cancer. The World Health Organization classifies it as a “white plaque of questionable risk,” necessitating the exclusion of other disorders. Various forms exist, with non-homogeneous types showing a higher risk for malignancy. Proliferative verrucous leukoplakia (PVL) is particularly aggressive, carrying transformation risks over 60%.
Affected individuals often include middle-aged and older adults, predominantly males, with tobacco use as a significant risk factor. Challenges in predicting which lesions will progress to cancer remain despite advances in understanding the molecular changes involved. Surgical excision is the primary management for higher-risk lesions, highlighting the need for surveillance and lifestyle changes to reduce recurrence and malignancy.
Diagnosis and Classification
To diagnose leukoplakia, distinguishing it from other white lesions in the oral cavity is essential, relying on clinical and histopathological evaluations. Clinically, leukoplakia can be homogeneous, appearing as a flat white patch, or non-homogeneous, with mixed color changes indicating higher malignancy risk. Biopsy results further aid in confirming the diagnosis and determining the presence of dysplasia or carcinoma.
Proliferative verrucous leukoplakia is a distinctive subtype that is more prevalent among older women and has a high transformation rate. Understanding the variant and location of leukoplakia can inform the management strategy moving forward.
Risk Factors and Causes
Tobacco consumption, whether smoked or chewed, significantly contributes to leukoplakia’s development, with a strong correlation between severity and duration of use. Alcohol often exacerbates risks when combined with these habits. Other factors include chronic irritation, fungal infections, and specific nutritional deficiencies, all of which can influence the condition’s onset and progression.
Moreover, demographic trends reveal a predominance in middle-aged males, especially in regions where smokeless tobacco is popular. Addressing and eliminating these risk factors can play a crucial role in managing and preventing leukoplakia.
Pathophysiology and Progression
Leukoplakia’s histological basis includes hyperkeratosis and dysplasia, the latter indicating a higher risk for malignancy. Dysplastic changes signal possible progression to carcinoma, with severity ranging from mild to carcinoma in situ. Factors impacting the microenvironment, such as immune cell interactions, also significantly influence dysplastic behavior.
Recent studies suggest that epigenetic markers, such as aberrant DNA methylation, may help identify high-risk lesions. Monitoring these changes offers insights into the potential for malignant transformation, reinforcing the importance of ongoing pathological assessment in affected individuals.
Management Strategies
Surgical intervention represents the mainstay treatment for leukoplakia, particularly with dysplastic lesions. Methods such as excision, laser therapy, and cryosurgery are prevalent, especially in high-risk areas within the oral cavity. Addressing lifestyle factors like tobacco and alcohol use is crucial for reducing recurrence.
Long-term monitoring is vital as leukoplakia can recur, especially without lifestyle changes. Comprehensive management may also explore adjunct therapies targeting inflammation and local irritants, though their effectiveness varies.
Prognosis and Outcomes
The transformation risk for leukoplakia can vary widely, influenced by factors such as lesion size and dysplastic degree. While most lesions remain benign, aggressive forms like PVL show significantly higher malignancy rates. Continuous monitoring and addressing modifiable risk factors are essential in reducing the likelihood of complications.
Research into biomarkers may enhance predictive capabilities, though much work remains to establish reliable indicators for individual patients. Regular follow-ups are critical in managing and detecting any malignant changes early on.
Prevention and Public Health Initiatives
Preventing leukoplakia is largely about reducing exposure to known risk factors, mainly tobacco usage. Educational initiatives aim to raise awareness and promote behavior changes within communities, particularly in high-risk populations.
Comprehensive strategies also stress the importance of early detection through regular oral evaluations and by addressing surrounding health factors like nutrition. Supporting cessation efforts and education on the condition can significantly impact overall public health outcomes.
The content is provided by Sierra Knightley, Front Signals